Telemedicine: Healthcare That's Virtually There
Thanks to high-definition video conferencing, fast network connections and the rising costs of hospital and patient visits, telemedicine use is on the rise. In fact, an August 2012 study, conducted by the research firm GlobalData, predicted that the worldwide telehealth and telemedicine market would grow at a compound rate of 14 percent between 2011 and 2018, reaching $32.6 billion.
“Increasingly, the point of patient care is moving from inside the walls of the hospital, which is the most expensive place to deliver care, to outside those walls,” says Kevin Boyle, business leader for Rubbermaid Healthcare, “Telemedicine is one of the major enablers making that happen.”
A major driver of the telemedicine market is the nationwide shortage of medical specialists, including radiologists, neurologists, dermatologists – and even primary care physicians – particularly in remote rural areas. These shortages will only grow more acute as the Affordable Care Act brings millions more potential insured patients into the national healthcare system.
What’s more, as virtual doctor visit services – connecting patients from their homes with physicians via online video – become more commonplace, insurers and employers are more willing to pay for them. Case in point: WellPoint Inc., the nation’s second biggest health insurer, recently announced plans to offer a new service, which allows people to consult with doctors using video-enabled devices.
Camera Caregiving
Telemedicine and telehealth is often used as a broader term to encompass health-related communication outside of clinical services. They embrace many types of long-distance healthcare solutions – for example teleradiology, telecardiology, even teledentistry – but can be broken down into the following broad categories:
Remote Monitoring
As they age, many people develop chronic medical conditions, such as diabetes, congestive heart failure and chronic obstructive pulmonary disease (COPD), which require constant monitoring and preventive care. Some studies have estimated that up to 75 percent of healthcare dollars are spent on chronic conditions that worsen with age.
Doctor’s office and emergency room visits are the most expensive ways to monitor and care for these chronic conditions. That’s why remote patient monitoring devices and software, which collect data from glucometers, blood pressure monitors, pacemakers and other monitoring devices at the patient’s home or elsewhere and send them to central monitoring systems for interpretation, are growing dramatically in use.
Not only does remote patient monitoring reduce the costs of chronic care, it has been shown to improve outcomes. Busy patients can be monitored more frequently to prevent emergency room visits; alerts can be triggered and sent to doctors, nurses or even first responders automatically when measurements exceed defined thresholds; and doctors and patients can look at graphical histories, medical advice and other valuable feedback. Reminders can also be sent to smartphones so patients don’t forget when it’s time to get a reading.
Remote patient monitoring has also moved into intensive care units. Here rural or other hospitals, that can’t afford internal 24-hour specialized intensive care visits, can take advantage of expert services that monitor patients’ vital signs remotely, often for many hospitals simultaneously.
There are also services for remote neurophysical brainwave monitoring during surgery.
“The person doing the monitoring may be a few doors down, in another hospital, sitting in a central monitoring center or even at home,” says Jonathan Linkous, CEO of the American Telemedicine Association. “I know of one case in which a traveling physician monitored an emergency surgery from his hotel room.”
Store and Forward
Lots of rural and smaller hospitals don’t have the funds to retain a full complement of in-house specialist pediatric, neuro- or musculoskeletal radiologists 24 hours a day, 365 days a year. Therefore, many take advantage of teleradiology to send or provide remote access for specialists at other network hospitals.
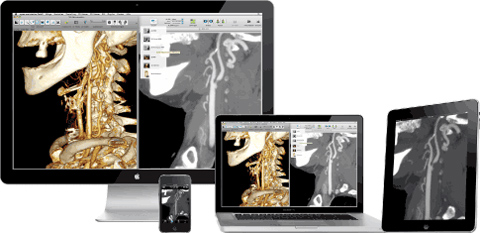
Some of these features are provided by specialized teleradiology systems and cloud services, with workflow applications that can queue up and securely send X-ray, CT or MRI images securely. In other cases, the function is provided by radiology information systems (RIS) and medical picture archiving and communication systems (PACS).
Recently, Aycan Medical Systems received an FDA 510(k) approval for a teleradiology app for the iPad, from which medical care specialists will be able to read CT and MRI images anywhere they happen to be. This type of store and forward technology is also used to send high-resolutions photos of skin conditions to remote dermatologists or wounds to other remote specialists.
Interactive
Perhaps the sexiest and emerging category of telemedicine, it uses everything from consumer PC and smartphone web cams to specialized mobile medical carts and high-definition telepresence systems for live, real-time video communication and healthcare. Consumer video chat applications or specialized health video services are increasingly being used for patient-to-doctor communications, particularly for remote mental health counseling.
“The VA hospitals often use web chat for post-traumatic stress disorder therapy,” says Linkous. “We estimate 300,000 to 400,000 patients see their therapists this way each year.” Traveling or less-mobile, older patients sometimes connect over live video with their primary care physicians or a nurse practitioner to address minor illnesses. Though in many areas there are medical licensing and insurance reimbursement issues that need to be addressed to make this more frequently used.
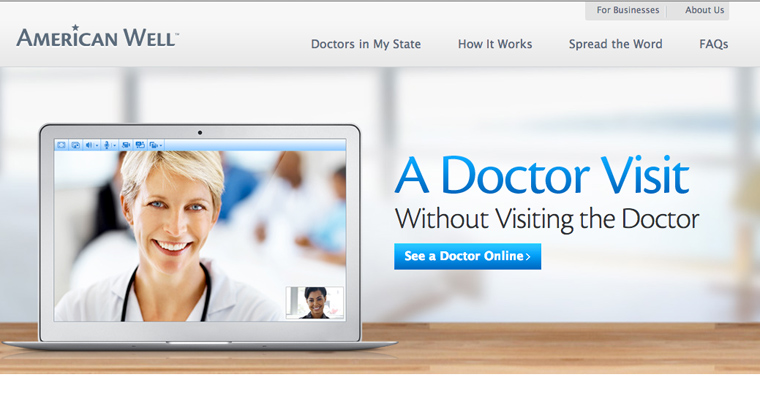
“In some parts of the country, a parent whose child has an earache can use online care services, such as those from telehealth company American Well, to find and connect with a pediatrician over live video,” says Lynne Dunbrack, program director, Connected Health IT Strategies for IDC Health Insights.
Insurance companies such as Blue Cross Blue Shield and pharmacy chains such as Walgreens are helping to provide these services in certain areas through services such as American Well. Hello Health has a similar service in the New York area that enables doctor visits via video and text chat and even email.
Doctor-to-Doctor Care
For doctor-to-doctor video consultations, there are more advanced and specialized video conferencing solutions available. For example, if a primary care physician or emergency room needs to consult with a neurologist, he or she may use one of several high-definition mobile or stationary video conferencing medical cart solutions from Cisco, Polycom, Rubbermaid or Vidyo to do so over live high-definition video.
This is a frequent practice when stroke is suspected. This not only brings in remote expertise that may not be available locally, it also provides a form of medical education for the primary care physician and perhaps the patient as well. And it can shave a lot of time off patient care.
These vendors offer specialized mobile multipoint video conferencing carts that provide not only high-definition, zoom-enabled video cameras, displays and graphics for realistic real-time video, but USB, VGA and other ports for plugging in medical monitoring, diagnostic and other devices. This allows remote healthcare providers to examine patients remotely and read diagnostic results live.
Telemedicine can also overcome geographic and budgetary constraints that stand in the way of face-to-face interactions. It can help patients to maintain closer contact with medical providers and reduce the need for staff travel, thereby saving cost and time.
Most experts agree that telemedicine is in its infancy and that mobile devices will enable many types of remote care solutions that haven’t even been imagined yet.
“Of course, there will always be the need for hands-on care and emergency room visits,” Boyle adds. “However, I think we’ll see telemedicine used for more and more patient care functions over the next five years as a complement to traditional healthcare.”










